The birth control pill. The contraceptive pill. Oral contraceptives. Magic pills. Mum’s Special pills. The pill is a plethora of names and identities.
Currently, women have the options of two types of pills. The combined and the ‘mini’, sometimes called a POP. Both contain synthetic versions of the hormone progesterone, but the combined is a cocktail including oestrogen too.
Time to dust off some GCSE biology knowledge to explain how these drugs work. Oestrogen stops the ovaries from releasing an egg and progesterone makes the uterus uninhabitable for sperm. Think of them both like bouncers at a club. Club Uterus is strictly invite-only, and sperm and eggs aren’t on the list.
Now, however, many women aren’t having their pill shaken, stirred, or even as a single. They’re going pill sober. Cold turkey. They’re breaking up with the pill.
NHS data reveals a decline in the use of the pill. In 2013, 48% of women used the little embryo embargo. 10 years later this figure had shrunk to just 27%. The numbers continue to jump lower.
A report, Contraception Re-Imagined, published by BPAS at the end of last year exposed the growing dissatisfaction. The numbers tell a striking story. 28% of women are not using any contraception at all. 12% of women are using the combined pill, with 9% using the mini. This means now only 21% of women use the contraceptive pill.
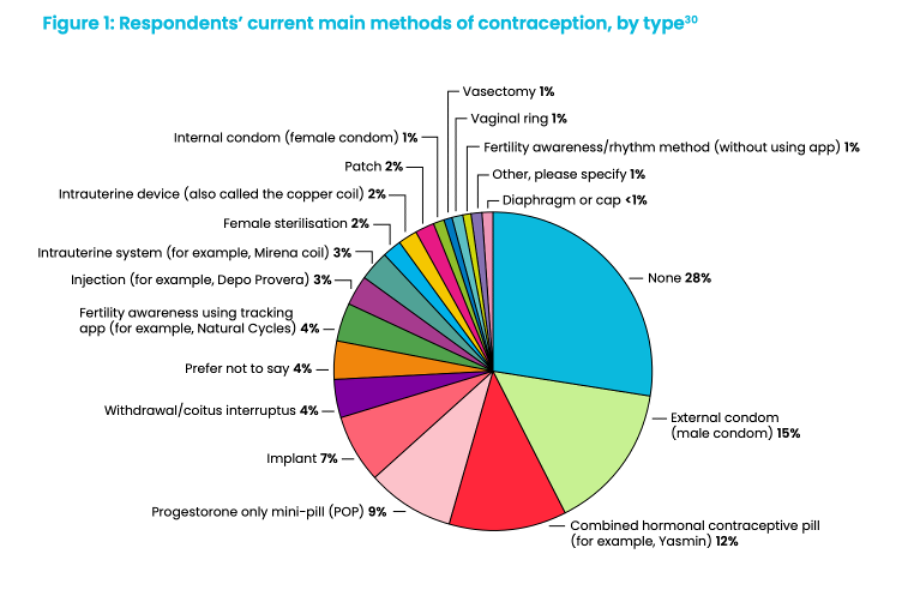
Photo: Contraception Re-imagined Report, BPAS
“Hormonal contraception is a conveyor belt for women. It’s often not personalised care,” Dr Rebecca Steinfeld, the writer of the report, tells me, “Contraception isn’t a one-size-fits-all.”
We’re meeting on zoom. Outside, it’s the time of year when the air has lost its crisp bite, replaced by a lingering chill. The gloomy, frosty morning contrasts Rebecca’s welcoming smile.
“There’s an incomplete data picture, we need to be careful not to overstate the impact of covid,” she replies after I ask whether women are moving away from the pill. “Something is apparent, though, that’s that women are turning away from hormonal contraception, especially the pill.”
Throughout our meeting it became clear. Rebecca wasn’t just the writer of the BPAS report. She was an activist who passionately believed in women’s rights.
BPAS also found there’s a new contraceptive on the block: Fertility Awareness Based Methods (FABMs).
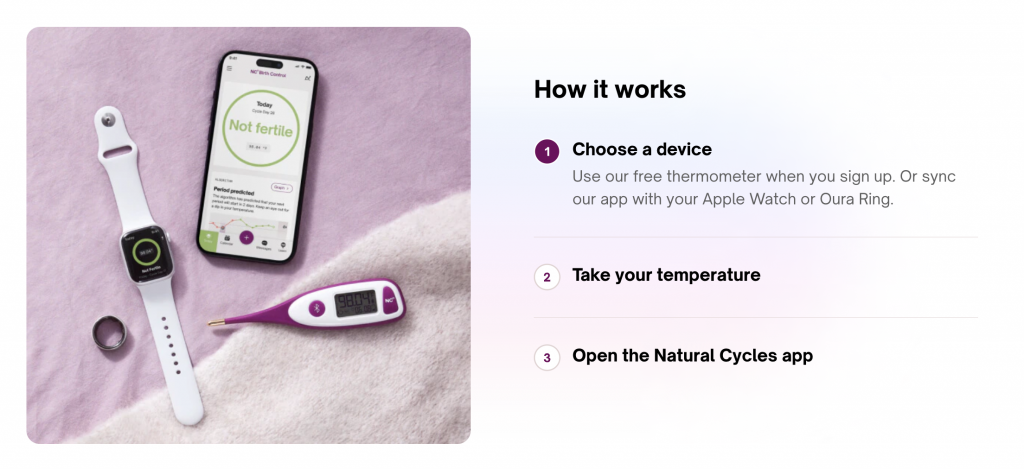
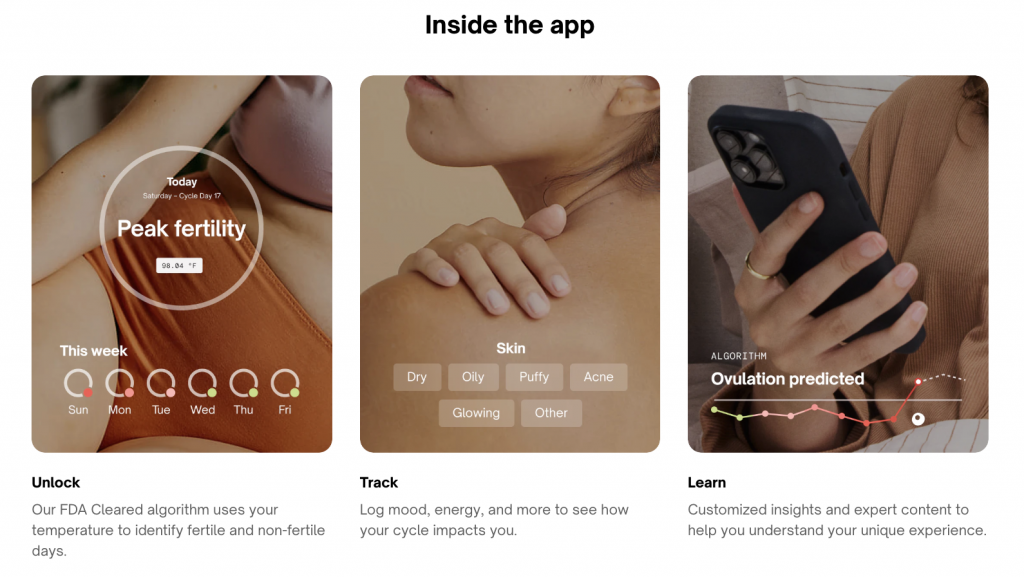
Photos: Natural Cycles
Once shunned as ‘the rhythm method’, FABMs have undergone a makeover thanks to technology. They rely on tracking ‘biomarkers’ like body temperature, urinary hormones, and cervical mucus through various devices. Users then input this data into an app or device where algorithms then predict high and low fertility days. When used as a contraceptive, users abstain or use barrier methods like condoms during fertile windows.
They’re getting popular too. Between 2018 and 2023 women using FABMs increased from 0.4% to 2.5%. In 2024 this figure is now 4%.
“Currently the app Natural Cycles, is the only FDA approved FABM” Rachel Peragallo Urrutia says. She’s an assistant professor in the Department of Obstetrics and Gynaecology at the University of North Carolina.
Because of the 3,888-mile distance between us, we’re meeting on Zoom, both framed by cloudy grey skies behind us. There, the afternoon is just beginning. Her sky still has the possibility of being greeted by sunlight. Here, ours was fading to black. The evening was stealthily creeping in.
She began researching FABMs back in 2013.
“I was interested in them myself actually, and often wondered ,‘who actually knows how to use these?’” she tells me on Zoom. As an OBGYN herself, that’s an Obstetrician and Gynaecologist for those of us who typically only see our GP, she had women coming to her as early as 2014 asking, “what can I use?”.
Natural Cycles has become a new contraceptive conquest for women who feel frustration with the pill. This existed long before but why are women breaking up with it in the first place? How did this relationship turn toxic?
The honeymoon period
Like most relationships, starting the pill feels like a honeymoon period.
Historically, honeymoons were in the pill’s DNA, or should I say, in its synthetic progesterone and oestrogen.
Seventy years ago, research into what would become the infamous ‘pill’ began. Contraception wasn’t a new idea. Using hormones was. In the 1920s, American Margret Sanger began her own research into hormonal ‘family planning’ methods. Beginning life as spermicides, a chemical that killed sperm, women’s hormonal contraception was uncharted territory.
Enter Dr Gregory Pincus. With his bushy moustache and prominent eyebrows, Pincus was recruited by Sanger. In 1953 he began his revolutionary work. Two years later human trials began in Puerto Rico. Women were tested on without informed consent. Coerced, controlled, and left in the dark. The trails’ murky ethics tainted the pill’s legacy with eugenics.
All was apparently forgiven, like a celebrity comeback after a well-timed apology, when the first birth control pill was approved by the FDA in 1960. Envoid. The Pill that changed the shape of women’s medicine and health forever.
With its FDA approval in hand, the pill made its way to Britain. Cased in pastel-coloured dialpak dispensers, the pill first hit prescription counters for married women in 1961. This gave the pill an official birth certificate. A British passport and visa for life.
Being on the pill was a members only club for women with a ring on their left hand until 1967. The NHS’s Family Planning act gave local health authorities permission to give birth control advice regardless of marital status. By 1974, it was available on the NHS for all women.
First, it was a married women’s luxury. In 1967 it was a women’s right. By 1974 it was an NHS staple.
Once it lost its exclusivity, it became more than a pill. It became a symbol. Tiny tablets wrapped in foil prescribed women to independence and sexual liberation. Once diamonds were a girl’s best friend. Now it was the pill.
Fast forward 50 years, this liberation is still felt.
Enovid bottle Photo: designKULTUR
Enter Viviana, a 20-year-old Nottingham graduate with cherry-red hair. I first met Viv backpacking the Balkans, with my trip coming to an end and hers just beginning in Corfu. Having bonded over cheap drinks and chats about love, boys, and heartbreak, we kept in contact over Instagram. 6 months later, she messaged me about this piece.
“I got the pill during covid so all of my appointments were over the phone,” she explained to me via voice note, “they asked me for my age and blood pressure… oh and why I wanted to be on the pill.”
And why did you want to be on it?
“My friends were on the pill, and I didn’t want to be irresponsible. I didn’t want to start having sex with no protection. As a fifteen-year-old it was exciting to be granted independence and the ability to control my own life in a way”
Liberation and Independence. It’s almost as if the spirit of the swinging sixties was right there with us.
For many women, the pill wasn’t just about sexual liberation, it was about liberation from painful debilitating periods. Especially for Zara.
“I was prescribed the pill Rigevidon, or whatever that stupid pink one is called, when I was 15 by a male doctor who couldn’t be bothered to actually look into my severe mood swings around my period.”
I’ve known Zara since childhood, when her bedroom walls were lilac and covered in One Direction posters. Harry, her childhood favourite, had the prime spot above her bed. Like a guardian angel.
“Oh, and a few evil eyes scattered around too,” Zara reminds me as we reminisce.
Now, she’s an almost 23-year-old woman. The lilac walls are gone, replaced by the neutral rented ones of her London flat. Some things haven’t changed though, evil eyes still claim their space. I wouldn’t be surprised if she had a Harry Styles poster tucked away somewhere too.
“I initially went to the GP for severe mood swings and anxiety around my period. I got put on the pill straight away, no questions asked. I wasn’t listened to by the male doctor. I felt like he didn’t care enough to find the root cause of the problem.”
But did it work? Did it help that?
“I feel like it worked but I think it was just masking the symptoms temporarily”
The red flags
Despite its fame, the pill has a few skeletons in its closet. Its risks.
In the late 1960s, a link between high levels of oestrogen in the pill and the risk of blood clots and stroke was being studied. Like a flock of chickens aware of a fox in the coop, women and their husbands were suddenly confronted by a danger they’d unknowingly been living with. By the 70s, the media picked up on these studies, sparking a frenzy.
As I scrolled through The Times online archive, searching for headlines for the pill in the 60s and 70s, I half expected to come across headlines celebrating revolution. I instead saw the sensationalised headlines from these once clueless, but now apparently headless chickens. I was greeted with headlines that read “Wife Who Took the Pill Dies,” “Blood Clot Kills Woman,” “What Women Risk by Taking the Birth Control Pill,” and “Birth Pill Killed Wife.” That’s just the tip of the Battenburg.
Rigevidon, the ‘stupid pink thing’ that Zara was prescribed, estimates that 5 to 7 women out of 10,000 will develop a blood clot in the first year of taking their pill. In fact, any combined pill containing levonorgestrel, a synthetic progesterone, comes with the same risk. Levonorgestrel isn’t the only blood clot culprit. Drospirenone, its synthetic brother, carries an even higher risk of blood clots, a risk that’s 3-4 times greater.
These synthetic progesterones, however, are only clot crooks when they work with their oestrogen sidekick. A 2012 study found higher doses of oestrogen in pills increase risks of blood clots and stroke. Pills like Microgynon, Gedarel 30 and Desogestral, all containing 30 micrograms of synthetic oestrogen, have a 6 times increased risk of stroke. Lower dose pills, like Millinette and Gedarel 20, carry an up to 3 times increased risk. It seems like oestrogen is a bad influence on progesterone.
To put this into perspective, Covid vaccinations had a 4 in a million risk of blood clots. Women who don’t take the pill face a 2 in 10,000 chance of developing a clot. It’s almost as if the combined pill cocktail is served with a game of Russian Roulette.
Rigevidon, the ‘stupid pink thing’ Photo: The Lowdown
“The ultimate fact is that women want transparent information and want to feel well informed.”
Working solo in progesterone only pills, progesterone carries no clot risk. Although, it’s not entirely free of dangers. These pills still carry the same cancer risks. Increasing the risk of breast cancer by 29%. You can take your halo off now, POP.
“The pill was originally used to treat endometriosis, but it wasn’t long before concerns over increased cancer risks and case reports of blood clots began to circulate in medical journals,” Lisa Iverson tells me, “Initially the cardiovascular risks were unexpected.” This explains the headless chickens.
Lisa is a smiley epidemiologist whose main interest is in women’s health. She manages the Royal College of General Practitioners’ Oral Contraception Study. The study, which began in 1968, follows 46,000 women who first took the pill to assess the long-term risks of the contraceptive pill.
Currently, she’s on my laptop screen. Her office is filled with research and paper. Behind her, post-it notes cover the walls.
“The risks of the pill are consistent,” she explains, “but these risks should be understood in absolute terms. They’re not absolute risks. There should be a personal understanding of the balance between risk and benefits.”
What about the cancer risks?
“While it does increase the risk of breast cancer, it actually, decreases the risks of ovarian and endometrial cancers. The pill’s protective effects against endometrial cancer can last for 30, even 35 years after discontinuation of the pill.”
In fact, oral contraceptives reduce the risk of endometrial cancer by 30%, lower ovarian cancer risk by up to 50%, and cut colorectal cancer risks by 15 to 20%. Suddenly, it seems the pill isn’t a game of Russian roulette after all.
The real problem doesn’t necessarily appear to be these risks, however.
“I had women coming to me as early as 2014 asking, ‘What can I use?’”
Ellie, a student from Devon, was prescribed the pill through a sexual health clinic when she was 17. As she sat in the clinical concoction of blues and whites on the walls and floors of the clinic, she was taken through the physical side effects. “Although we went through many physical side effects, at no point was I made aware of the mental side effects,” she tells me, “The main reason I stopped was because I developed depression and then OCD.”
And would you have tried it if you had been told?
“No.”
For Ellie, it’s as if the sterile environment had sterilised the conversation itself.
Similarly ,Grace, 23, was prescribed the pill without any information on the side effects. Until she was 14, she missed school once a month due to the severe pain of her period. With the classroom being replaced by sick buckets in her bedroom every month, her dad took her to the doctor. She was prescribed the pill. A seven-year relationship started.
“I wasn’t aware of the side effects at all at 14. They weren’t discussed at the time of it being prescribed, I was sold a dream.”
For seven years, Grace battled a minefield of depression, weight changes and loss of libido without knowing the cause. “Now I know it was because of the pill”, she tells me, “Now I know its side effects, I’m angry at the doctor for putting such a young girl on the pill,”
Like the big bad wolf dressed up as granny, the pill was dressed up as Grace’s hero.
The problem, it seems, lies with how doctors communicate risks. Risks, including side effects. The same deception that women felt in their bellbottoms of the 70s is felt by women in their slick-back ponytails of the 2020s. It’s as if the miscommunication has its own cycle, just like periods an d pills themselves.
“Contraception is feelings based,” Dr Rose Stevens says, “it’s not one size fits all.”
When she’s not chatting to me on zoom, Rose is a researcher in the Institute for Women’s Health at UCL. She’s currently working with the Department of Health on a study exploring why women are moving away from contraception and what can be done to address it.
“Yes we are seeing women break up with hormonal contraception,” she tells me, her face illuminated by the glow of her laptop screen, “the prescription of pills and fittings of IUDs have decreased, for example, but we cannot ignore the impact of covid and the accessibility of abortions.” London is faintly humming through her open window.
“Depending on our findings, we’ll produce materials for doctors and sexual health practitioners to help women make better-informed decisions.”
Her research could change the future of reproductive health medicine, ensuring that women make informed choices and access contraception suitable for them. Care that considers the needs of women like Grace and Ellie.
The relationship has turned toxic. What women are told when they’re first prescribed the pill and, more importantly, what they’re not, haunts women and their relationships with these Womb Bouncers.
Yet, despite the risks and the silent tiptoe around them, only 16% of women actually change their contraception because of these concerns. So, what else is this knight in shining armour hiding?
The breakup
Alice Pelton, the founder of The Lowdown, may not know where Sir Pill keeps its secrets, but she knows about women’s real-life experiences with it. If you haven’t heard of The Lowdown, let me give you the lowdown. With 80% of women getting side effects from their contraception, Alice was keen to set up a website where women could choose and access the right contraception for them. And so, The Lowdown was born, a website that does just that, and so much more.
“I noticed dissatisfaction around 8-10 years ago. I like to think the lowdown was ahead of its time,” Alice chuckles in a voice note to me while hopping on a red London bus, “a lot of the stories we’ve seen in the media are something we’ve known and have been saying for years and years. It’s not new news.“
I first got in contact with Alice on LinkedIn. Scrolling through the site, as most soon-to-be graduates do, I saw her post. After seeing news stories covering the link between abortion rates in the UK and FABM, she wanted to talk to journalists on why women were moving away from the pill in general.
Enter, me, stage left.
‘These ‘breakups’ shouldn’t over overstated,” she says, “150 million women worldwide are still using the pill, so that’s only a tiny percentage of women using Natural Cycles and other fertility awareness-based methods,” a car horn honks in the background.
“I knew I had to break up with it,” says Ersi, 23. She’s one of the few not among the 150 million women still using the pill.
Were sat in a coffee shop. Our coffee shop. The one we used to work at together. The walls are a shade of blue that matches the railings on Tower Bridge, which is just a short walk away. Were sat opposite each other, both sinking into our leather armchairs.
After having a surgical abortion, Ersi was prescribed the pill. “I remember walking into the doctor’s office after the procedure, still feeling awful, both physically and emotionally. I can’t forget the way he spoke to me as he explained why I should start taking the pill,” She tells me, “he didn’t listen, not really. There was no understanding, no kindness.”
After gaining 15kg on the pill, Ersi realised it was time for a breakup.
Did you know that was a side effect? I ask as she took a sip from her oat cappuccino, no chocolate. “Yes, the doctor did explain the side effects to me, but honestly, I didn’t really pay much attention or feel bothered by them at the time. The way he was speaking to me made it hard to focus, it felt so dismissive and rushed. I just kept nodding and saying, ‘yes, yes, yes’.”
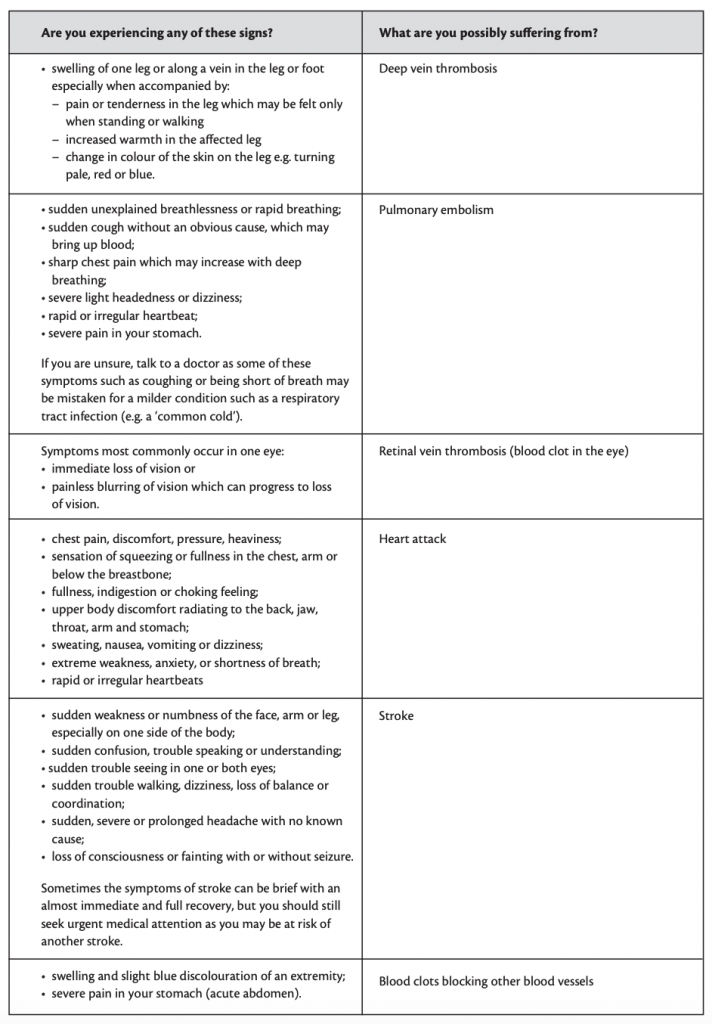

Rigevidon side effect leaflets

The pill is a pandoras box of side effects.
Rigevidon, one of the UK’s most prescribed combined pills, lists 63 possible side effects in its ‘user manual’. The manual itself is so big it could double as a blanket. For comparison, Tesco Ibuprofen has 21. Given that it’s the size of a dish cloth, it’d also be a pretty useless blanket. Unless, of course, you were the size of a Barbie.
“The Lowdown focuses on five key side effects where the pill gets the most criticism: mood, skin, weight, periods, and libido.” I’m back on a London bus with Alice, I can hear the familiar sound of the bus door closing, repetitive and high-pitched like the beep of an alarm clock.
On their website, that looks like a homage to Trip Advisor, the combined pill has over 2,500 reviews with an average rating of 2.8. As I scroll through the reviews, the frustration fills my screen. The side effects cannot escape being mentioned, even among the most positive reviews. Women’s dissatisfaction hits me like a tidal wave.
It was an exposé.
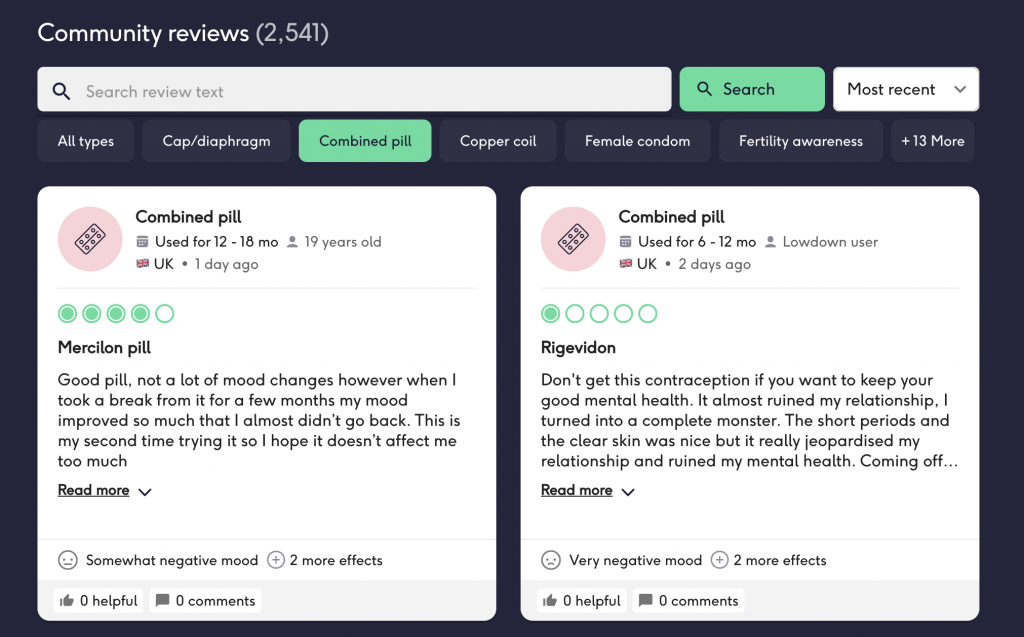
Review page on The Lowdown Photo: The Lowdown
Out of the ten most recent reviews, six mention a negative effect on mental health. These side effects range from low mood and anxiety to depression and suicidal thoughts. The pill wasn’t just harmful to physical health, but mental too.
Buried within the small print of the blanket-cum-user manual, these mood changes are listed. It is a member of the ‘most common’ side effect club, affecting 1 in 10 women. Studies, however, found 58% of women report the pill to negatively affect their mental health in some way. What is the real figure the manual seems to be hiding?
“On reflection now, I don’t think I was given the right pill,” Miriam, 21, says to me, “my mental health suffered. I didn’t feel myself. I was negative all the time and looked at things in a negative light, it threw me off.”
This horrible feeling of disconnect from yourself was also felt by 21-year-old Riana who told me, “There were days where I couldn’t get out of bed.”
Stuck in her run-down university halls, Riana would look at the worn notice board, decorated by photos where she was smiling, happy. “I couldn’t spend time with friends. I couldn’t do uni work. I was in a low mood a lot more frequently on the pill.” The photos on that noticeboard were the only reminders if a version of herself she felt she lost due to the pill.
In 2017 Digital media brand The Debrief launched an investigation, Mad About the Pill. It found that 45% of women experienced anxiety and/or depression, with 20% of women suffering panic attacks. Just a year before, a Dutch study found women using hormonal contraception were also more likely to be prescribed antidepressants. Those on the combined pill are 23% more likely, while those on the progestogen-only pill face a 34% higher chance. Alarmingly, this is even higher for girls aged 15-18, with an 80% increased likelihood.
Ultimately, the side effects aren’t just a minor inconvenience, they’re a disruptive force in women’s lives. With 27% of women choosing their contraception specifically to avoid negative side effects, it’s clear just how significant their impact is.
The side effects are women’s Mount Vesuvius, erupting without waring and burying them under a thick layer of unwanted ash of depression, weight gain, loss of libido, blood clots, acne, stroke, breast cancer, nausea, headaches… need I go on?
Women are fleeing their side effect disaster. They’re breaking up with the pill.
Moving on
Like all breakups, whether they be good or bad, there eventually comes a time when singing Kelly Clarkson’s Since U Been Gone isn’t enough. The anger has gone. Tears dried up. Denial is now just a river in Egypt. There’s no more bargaining with other contraceptive methods. It’s time to move on. When it comes to the pill, this is no easy fleet. You can’t just hop on a contraceptive version of Hinge, Tinder or Bumble and swipe through all the possible rebounds. There are none. They all contain hormones or carry the same risks. Two of women’s apparent non-negotiables.
It’s not all doom and gloom, though. The BPAS’s Contraception Reimagined report unveiled two new promising non-hormonal options that are currently in the works. Cue the applause! Could women’s ultimate contraceptive solution finally be on the horizon?
One such alternative is contragestives, known as ‘late period pills’ in the U.S. These pills are taken after unprotected sex, after a missed period, or at any point in the cycle. They contain mifepristone, which, when used with misoprostol, together make up medical abortion pills. Currently, research is underway to test their use independently as a contraceptive. Rebecca Gomperts, founder of Women on Waves and lead researcher into these pills, describes them as either contraception, emergency contraception or abortion medication. I hope there’s an option for multiple identities on contraceptive Hinge.

The contragestive pill Photo: Women on Waves
Not only is it a safe and effective alternative to the pill, but it also won’t cause women depression or increase their risks of cancer or a stroke. Previous research suggests 1 in 20 women may experience side effects of nausea, headache, and fatigue. But, because neither oestrogen nor progesterone are in these late period pills, none of the nasty side effects occur. Phew.
These pills are attractive to women too. In 2015, 48.8% of women would use contragestives, 10 years later this figure is now 72%. It’s an instant Swipe right and match.
However keen women may be, though, research is being prevented by a law that predates the American civil war and the Merry-Go-round.
The 1861 Offences Against the Person Act prevents their legal classification. This is the same law that makes abortion illegal if the ‘rules’ of the 1967 Abortion Act aren’t followed. Due to this law and the nature of the drug, any medication that might disrupt a pregnancy after implantation may constitute a criminal offence. Boo.
Back on our bear hunt we go.
The other alternative contraception making waves is male contraceptives.
The first phase of clinical trials has already concluded for self-administered gels. Containing testosterone and progestogen, they prevent men from producing sperm. “Oh the phone was ringing off the hook,” Richard Anderson from the Anderson group that researches male contraceptives tells me. “It was quite surprising actually because women loved the idea of it more, if anything.”
He’s correct. The BPAS report found over three quarters of women would be open to their partner using this method.
We sit on zoom. He’s in a country cottage. I’m in a mould and mice riddled student house. His background hasn’t been blurred so I try and suss out the locations of the two prints behind him. They look like old prints of cities.
What are the hurdles then? If it’s being well received and no law is stopping it, then what is?
“Funding.” Deadpan.
Although his research is currently being funded by the American National Institute for Health, funding remains a major barrier for any new contraceptive.
A 2024 study in the Contraception Journal found that contraceptive research is severely underfunded. Only $149 million is invested annually in the US, below the estimated $500 million to $1 billion needed to drive innovation. In the UK, magazine Elle found that just 2.1% of public research is dedicated to reproductive health, with less than 1% of private funding and under 2.5% of public funding going to women’s health.
Women are at a loss. They hate their weight gain, bad skin, and loss of libido. They resent the depression, panic attacks and anxiety. They’re scared of the blood clots, stokes, cancer. But what they fear more? The unwanted pregnancy.
With funding and legalities preventing the coronation of a new contraceptive queen, when women aren’t relying on condoms or simply nothing at all, they’re increasingly turning to FABMs.
“Now i know the side effects… I’m angry at the doctor for putting such a young girl on the pill”
I’m back with Rachel in gloomy North Carolina. My sky had quickly turned black, hers is very much the same. Although, I wasn’t holding out much hope the sun would make an appearance for her either that day.
So why are women breaking up with the pill? And why are they turning to FABMs?
She leans back in her chair. There’s a slight awkward silence that I wait for her to fill.
“Ultimately, its frustration with the side effects of hormonal contraception,” she says in her American Accent, “the medical community tends to downplay them. I even learned how to dismiss them myself.” It makes sense. FABMs have no physical side effects, they’re also affordable and cost free.
This frustration, both by the dismissal of the medical community and the pill itself speaks to a deeper truth. “The ultimate fact is that women want transparent information and want to feel well informed” Rachel tells me before we say our goodbyes and exchange well wishes.
The pill is showing its true colours. Red ones. Like a red flag warning on a beach, women are no longer taking a dip in contraceptive waters. Fed up with its risks, side effects and misinformation, women are breaking up with the pill.